Clearly, the COVID-19 pandemic poses significant challenges for doctors and hospitals. For example, there are major capacity management issues and it possibly very hard choices will have to be made whether to treat a patient or not with only limited prognostic parameters available.
At Holland AI, we have been contemplating various avenues to offer non-profit support. We have added new functionalities to our application for detection of pulmonary nodules, analyzing the extent of lung damage by COVID-19.The main opinion of our team was that we should not engage in developing COVID-19 solutions unless we had the feeling that we could add real value to the scientific work being done on the pandemic. Also, we explicitly don’t want to leverage this crisis for commercial stakes.
Several algorithm vendors have developed (or are developing) algorithms for detection of COVID-19 on chest-CT scans or X-ray images of the chest. These solutions can definitely add value in situations where there is scarcity of radiologists in combination with a high volume of CT-scans.
However, in the Netherlands scarcity of radiologists is – knock-on-wood – not a problem at this moment. In addition, CT-features of COVID-19 are highly aspecific and can also be found in, for example, other types of pneumonias, and it remains unclear if an AI-tool can distinguish pneumonias based on their causative pathogen.
So, where can we add value using AI in this situation? As mentioned before, treatment decisions must be made and there are only a few prognostic parameters available. Several studies have used the so-called CT-severity score to make an estimation of the affected lung tissue in each lung lobe. One can imagine that patients with only 5% affected tissue may have a better prognosis than a patient with 50% damage, presenting on the same day after the onset of complaints. Dutch radiologists are currently reporting this score in the standard COVID-19 reporting template. However, this is an additional task in the ever-growing list of radiologist’s tasks and time-consuming in terms of assessment and reporting.
In addition, the CT-severity output can be used for integration in predictive models using other input data (e.g. blood samples and clinical parameters). In this way, the CT-severity score can important value for doctors (e.g. ICU-doctors and pulmonologists) to decide on the follow-up of treatment.
Considering this, we have decided to tweak and adjust the advanced segmentation capabilities of PulmoFast (our in-house algorithm for detection of pulmonary nodules), and deploy a model to provide quantification of the CT-severity score. The first version of this solution was built in only one week and we are very grateful for the tremendous teamwork. Of course, this is the first version and we are currently fast-tracking a development study in one of our main partner institutions (Maasstad Ziekenhuis Rotterdam). We will offer an API solution for all hospitals in the EU to use this tool free of charge.
How it works:
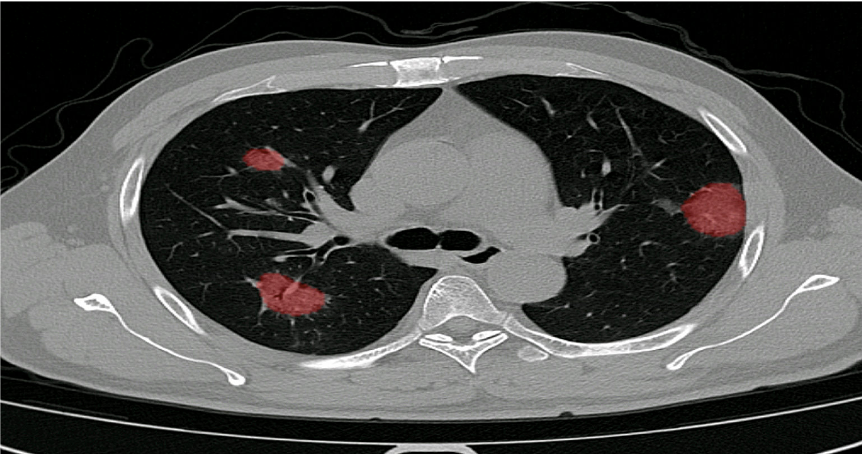
Automated scoring of the extend of damage inflicted on the lung due to COVID-19.
Scoring is shown per individual lobe, consistent with the scores used in numerous clinical studies
Fully integrated into existing workflow and PACS viewer.
Why do we do this from a developer’s point of view? To prove ourselves that we can develop such a solution within 2 weeks, with easy implementation, in full compliance with all relevant law and legislation. And after the crisis, we are happy to talk about how we can help your institution during ‘normal’ times with improving healthcare by deploying AI and machine learning.
When I first told people I wanted to become a radiologist, they all looked at me if I was going to embark on the Titanic. Very often I’m asked if I’m not afraid that the field of medicine I work in will be replaced by artificial intelligence in a few years. The answer is no. In fact, being a radiology resident, I’m highly excited about the potential that the field of radiology has for redefining the future of healthcare. Currently, this medical specialism is one of the first to start implementing and developing AI tools to improve the accuracy and speeds of diagnostics. This is highly necessary because of the enormous and exponentially increasing amount of radiology exams that are being made nowadays. Luckily, a lot of smart teams, universities and companies are busy building tools to reduce the workload of radiologists, to ensure the high-quality standards of diagnostics we all rely on.
There is only one strange thing I noticed. Hundreds of AI solutions have already been developed, but only a few make their way to clinics and above that, the majority has not shown to change care for patients. I started to incentivize what are the obstacles and found that there are many. However, the main obstacle is a lack of alignment between industry and hospital staff. So this was inspiring. What if we could just turn things around and start from scratch?
Together with my former study friend Damiaan Sprenger and a team of highly talented #AI developers we started building a platform for cloud-based AI implementation: #Holland AI.
We have launched our first application (PulmoFast) in the Maasstad Hospital in the city of Rotterdam (i.e. the best city in the world). From day 1 we talked and worked with all the hospital staff involved in the implementation (i.e. doctors, radiographers, IT-staff, physicists, legal officers, security officers, and so on). This approach has been instrumental in rapid deployment, and co-creation.
Also, we had great knowledge of support from #Microsoft. This eventually resulted in an implementation study of our algorithm for the detection of pulmonary nodules (potential precursors of lung cancer), which we call the #PulmoFast algorithm.
We expect to publish results of PulmoFast soon. Tip of the veil: it works pretty well! We are working on a bunch of other exciting projects at this moment, and we can’t wait to share developments with you on LinkedIn.If you’re interested in our activities, feel free to reach out to me on Linkedin!